Bipolar Disorder:
Definition:
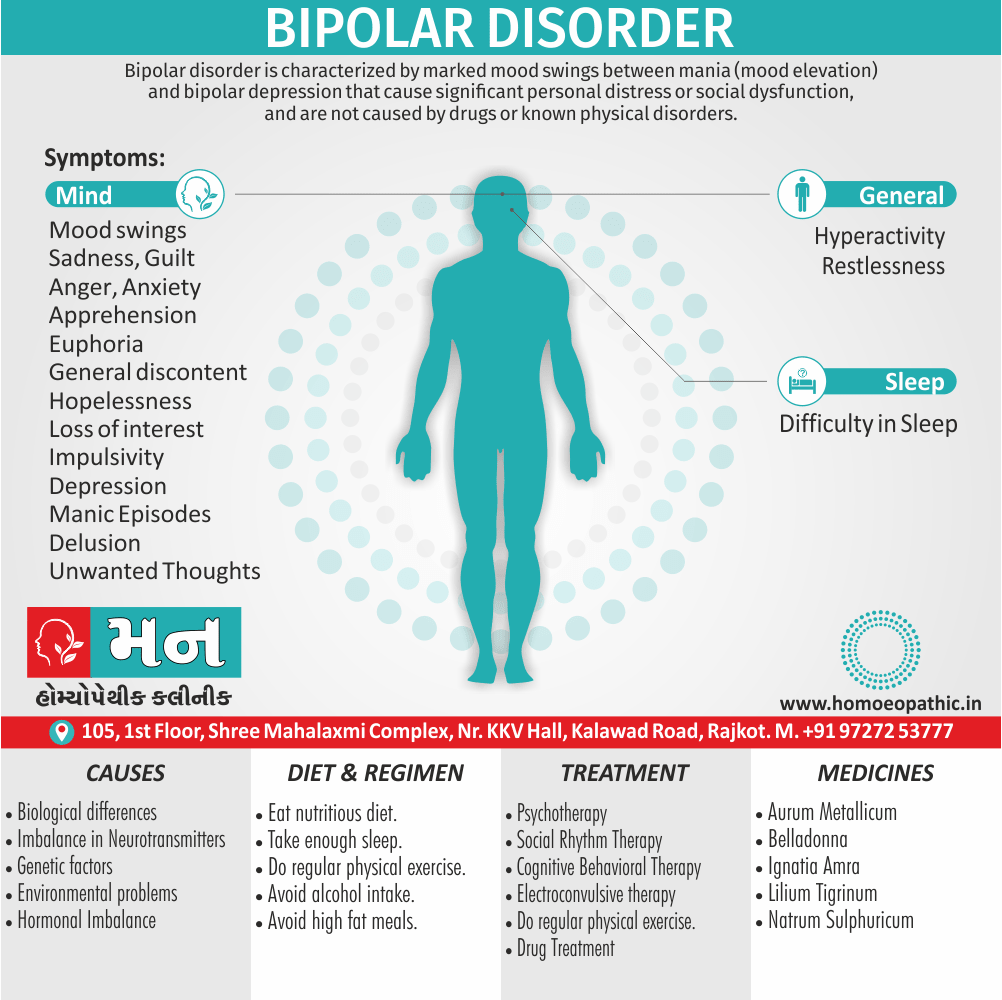
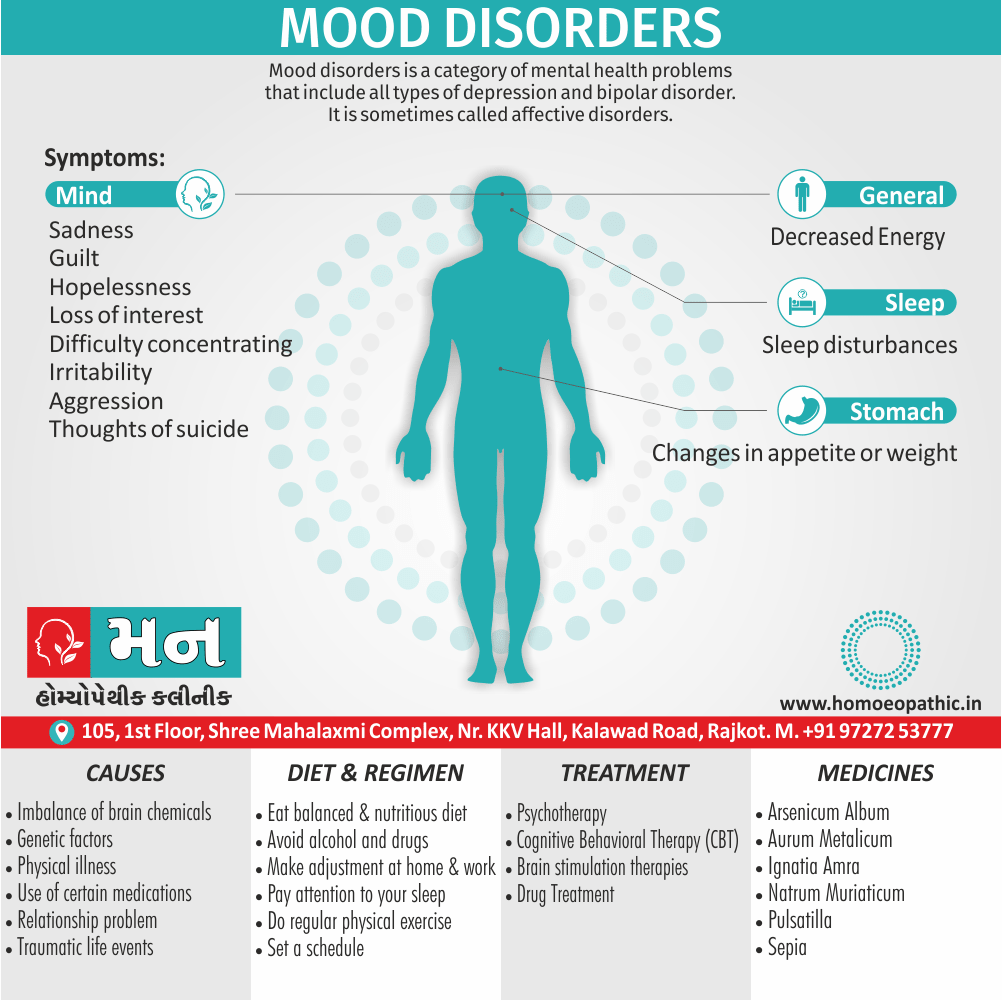
Bipolar disorder ( bipolar affective disorder, manic depressive disorder) is characterized by marked mood swings between mania (mood elevation) and bipolar depression that cause significant personal distress or social dysfunction, and are not caused by drugs or known physical disorders.
Bipolar disorder:
This disorder, formerly called manic depression, causes extreme mood swings that include emotional highs (mania or hypomania) and lows (depression). When you become depressed, you may feel sad or hopeless and lose interest or pleasure in most activities.
When your mood shifts in the other direction, you may feel euphoric and full of energy. Mood shifts may occur only a few times a year or as often as several times a week.
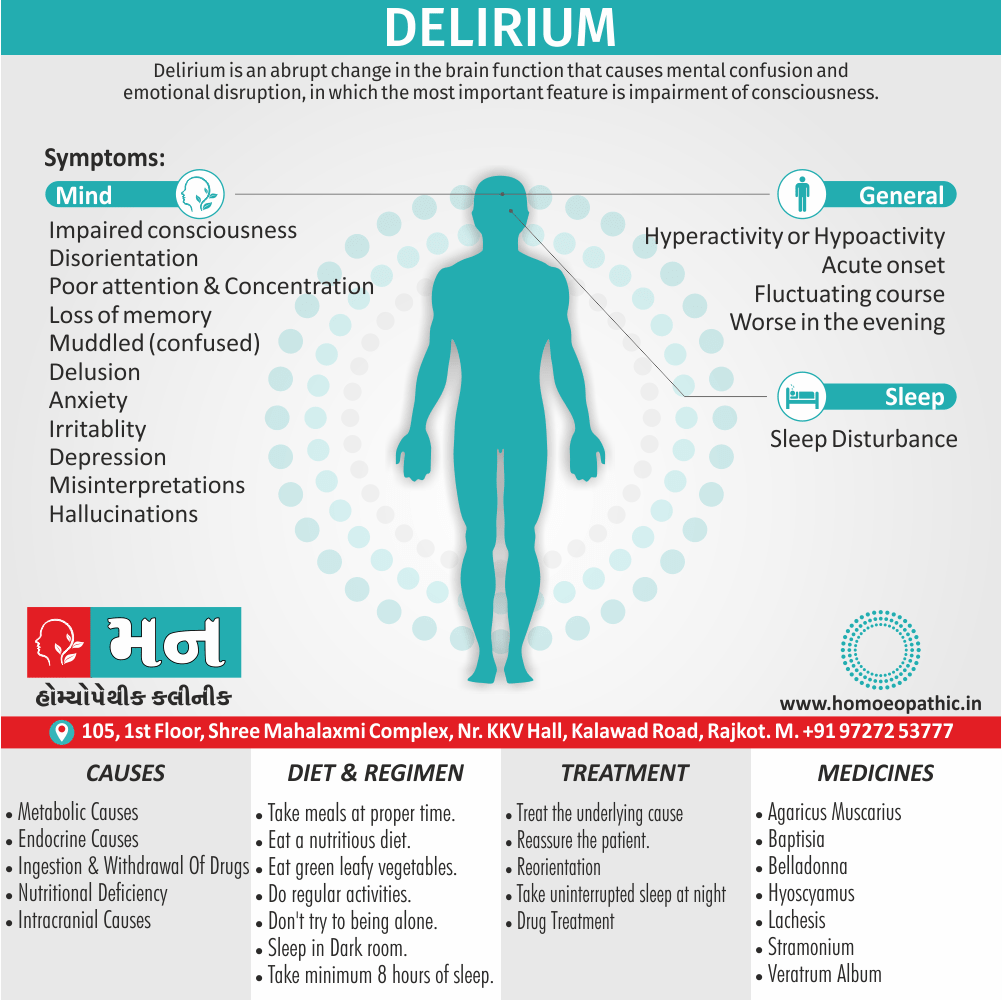
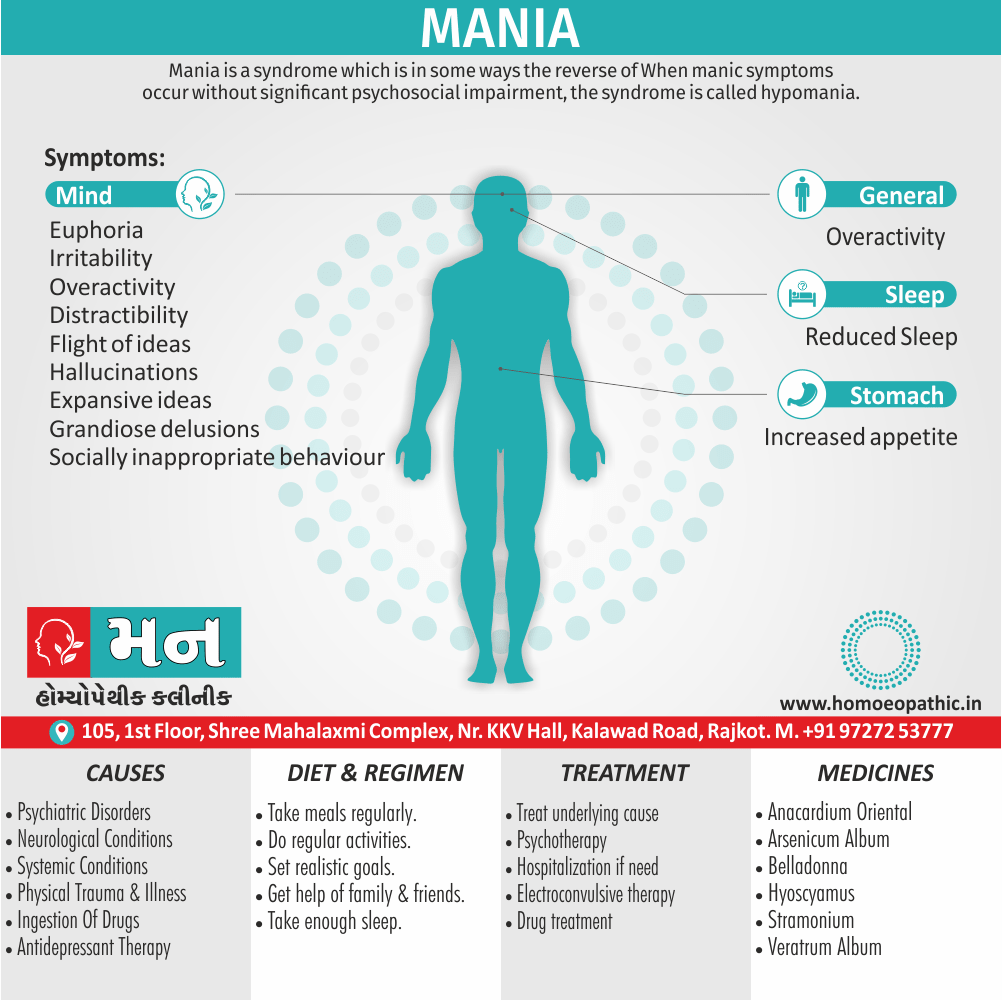
Mania:
Mania, a syndrome which is in some ways the reverse of depression, occurs as part of bipolar disorder. The term bipolar disorder implies episodes of both mania and depressive disorder, but the diagnostic category also includes those who, at the time of diagnosis, have suffered
only manic illnesses (most patients with mania eventually develop a depressive disorder). When manic symptoms occur without significant psychosocial impairment,
the syndrome is called hypomania.
The features of mania are;
- elevated mood,
- overactivity,
- and poor judgement.
Mania occurs as part of bipolar disorder in which there may also episodes of depression.
Mania is considerably less common than depressive disorder; it is important that mania recognize in its early stages because in the later stages the patient becomes increasingly unwilling to accept treatment. Long-term maintenance drug treatment to prevent relapse should considere in the management of patients with recurrent bipolar illnesses.
- The exact cause of bipolar disorder is unknown, but several factors may be involved, such as:
- Biological differences. People with bipolar disorder appear to have physical changes in their brains. The significance of these changes is still uncertain but may eventually help pinpoint causes.
- Neurotransmitters. An imbalance in naturally occurring brain chemicals called neurotransmitters seems to play a significant role in this disorder and other mood disorders.
- Inherited traits. Bipolar disorder is more common in people who have a first-degree relative, such as a sibling or parent, with the condition. Researchers are trying to find genes that may be involved in causing bipolar disorder.
- Factors that may increase the risk of developing this disorder or act as a trigger for the first episode include:
- Having a first-degree relative, such as a parent or sibling, with bipolar disorder
- Periods of high stress
- Either Drug or alcohol abuse
- Major life changes, such as the death of a loved one or other traumatic experiences
Pathophysiology of Bipolar disorder
- It is characterized by dysregulation in the dopamine and serotonin systems and by pathology in the brain systems involved in regulating emotion.
- Psychosocial stressors, notably life events and familial expressed emotion, significantly influence the course of the illness in the context of these vulnerabilities.
Types of Bipolar disorder
- Bipolar I disorder- involves periods of severe mood episodes from mania to depression.
- Bipolar II disorder- is a milder form of mood elevation, involving milder episodes of hypomania that alternate with periods of severe depression.
- Cyclothymic disorder- describes brief periods of hypomanic symptoms alternating with brief periods of depressive symptoms that are not as extensive or as long-lasting as seen in full hypomanic episodes or full depressive episodes.
- "Mixed features" – refers to the occurrence of simultaneous symptoms of opposite mood polarities during manic, hypomanic or depressive episodes. It’s marked by high energy, sleeplessness, and racing thoughts. At the same time, the person may experience hopeless, despairing, irritable, and suicidal feelings.
Rapid-cycling- is a term that describes having four or more mood episodes within a 12-month period. Episodes must last for some minimum number of days in order to be considered distinct episodes. Some people also experience changes in polarity from high to low or vice-versa within a single week, or even within a single day, meaning that the full symptom profile that defines distinct, separate episodes may not be present (for example, the person may not have a decreased need for sleep). Sometimes called "ultra-rapid" cycling, there is debate within psychiatry as to whether this phenomenon is a valid or well-established feature in bipolar disorder. A pattern of rapid cycling can occur at any time in the course of illness, although some researchers believe that it may be more common at later points in the lifetime duration of illness. Women appear more likely than men to have rapid cycling. A rapid-cycling pattern increases risk for severe depression and suicide attempts. Antidepressants may sometimes be associated with triggering or prolonging periods of rapid cycling. However, that theory is controversial and is still being studied. (2)
Conditions that commonly occur with bipolar disorder:
If you have this disorder, you may also have another health condition that’s diagnosed before or after your diagnosis of bipolar disorder.
Such conditions need to diagnose and treat because they may worse existing bipolar disorder or make treatment less successful. They i.e.:
- Anxiety disorders: For Examples include social anxiety disorder and generalized anxiety disorder.
- Post-traumatic stress disorder (PTSD): Some people with PTSD, a trauma- and stressor-related disorder, also have this disorder.
- Attention-deficit/hyperactivity disorder (ADHD): ADHD has symptoms that overlap with this disorder. For this reason, this disorder can be difficult to differentiate from ADHD. Sometimes one is mistaken for the other. In some cases, a person may be diagnosed with both conditions.
- Addiction or substance abuse: Many people with maniac disorder also have alcohol, tobacco or drug problems. Drugs or alcohol may seem to ease symptoms, but they can actually trigger, prolong or worsen depression or mania.
- Physical health problems: People diagnosed with this disorder are more likely to have certain other health problems, such as heart disease, thyroid problems or obesity.
Clinical examination:
Bipolar disorder is characterized by periods depression that alternate with periods of mania. Physical examination of patients with bipolar disorder is usually normal. A mental status examination physical examination should assess patients for
Major depression for 2 weeks being either a depressed mood or loss of pleasure, and presence of at least five of the following symptoms:
- Depressed mood
- Markedly diminished interest in nearly all activities
- marked weight loss or gain or significant loss or increase in appetite
- Hypersomnia or insomnia
- Psychomotor retardation or agitation
- Loss of energy or fatigue
- Feelings of worthlessness or excessive guilt
- Decreased concentration ability
- Preoccupation with death or suicide.
Mania: feature at least 1 week of profound mood disturbance, characterized by elation, irritability, or expansiveness and at least 3 of the diagnostic criteria
- Grandiosity
- Diminished need for sleep
- Excessive talking
- Racing thoughts
- Clear evidence of distractibility
- Increased level of goal-focused activity at home, at work.
- Excessive pleasurable activities.
- Hypomania characterized by an elevated, or irritable mood of at least 4 consecutive days duration. for diagnosis it require at least three of the symptoms of mania.
- Impulsive or risk-taking behaviors
- Suicidal thoughts and behavior
- Risk factors for suicide attempts and deaths.
- In addition to current symptoms, it is important to ascertain the number, frequency, intensity, and duration of past mood episodes.
Examination using the Mental Status Examination as well as assessment of the following:
- Appearance
- Affect/mood
- Thought content
- Perception
- Suicide/self-destruction
- Homicide/violence/aggression
- Judgment/insight
- Cognition
- Physical health
Investigation of Bipolar disorder
- There are no specific blood tests or brain scans to diagnose bipolar disorder.
- May perform a physical exam and order lab tests, including a thyroid function test and urine analyses.
Diagnostic criteria for bipolar and related disorders are based on the specific type of disorder:
- Bipolar I disorder: You’ve had at least one manic episode. The manic episode may be preceded by or followed by hypomanic or major depressive episodes. Mania symptoms cause significant impairment in your life and may require hospitalization or trigger a break from reality (psychosis).
- Bipolar II disorder: You’ve had at least one major depressive episode lasting at least two weeks and at least one hypomanic episode lasting at least four days, but you’ve never had a manic episode. Major depressive episodes or the unpredictable changes in mood and behavior can cause distress or difficulty in areas of your life.
- Cyclothymic disorder: You’ve had at least two years — or one year in children and teenagers — of numerous periods of hypomania symptoms (less severe than a hypomanic episode) and periods of depressive symptoms (less severe than a major depressive episode). During that time, symptoms occur at least half the time and never go away for more than two months. Symptoms cause significant distress in important areas of your life.
Criteria for a manic or hypomanic episode:
The DSM-5 has specific criteria for the diagnosis of excited and hypomanic episodes i.e.:
- Firstly, A manic episode is a distinct period of abnormally and persistently elevated, expansive or irritable mood that lasts at least one week (or less than a week if hospitalization is necessary). The episode includes persistently increased goal-directed activity or energy.
- Secondly, A hypomanic episode is a distinct period of abnormally and persistently elevated, expansive or irritable mood that lasts at least four consecutive days.
Criteria for a major depressive episode:
- The DSM-5 also lists criteria for diagnosis of a major depressive episode:
- Five or more of the symptoms below over a two-week period that represent a change from previous mood and functioning. At least one of the symptoms is either depressed mood or loss of interest or pleasure.
- Symptoms can be based on your own feelings or on the observations of someone else.
Differential diagnosis of Bipolar disorder
- Major depressive disorder
- Cyclothymic disorder
- Psychotic disorders
- Anxiety disorders
- ADHD
- Personality disorders (4)
Treatment of Bipolar disorder
- Psychotherapy
- Social Rhythm Therapy
- Cognitive Behavioral Therapy
- Electroconvulsive therapy
- Do regular physical exercise
- Drug Treatment
Homeopathic Treatment of Bipolar Disorder
Homeopathy treats the person as a whole. It means that homeopathic treatment focuses on the patient as a person, as well as his pathological condition. The homeopathic medicines selected after a full individualizing examination and case-analysis.
Which includes
- The medical history of the patient,
- Physical and mental constitution,
- Family history,
- Presenting symptoms,
- Underlying pathology,
- Possible causative factors etc.
A miasmatic tendency (predisposition/susceptibility) also often taken into account for the treatment of chronic conditions.
What Homoeopathic doctors do?
A homeopathy doctor tries to treat more than just the presenting symptoms. The focus is usually on what caused the disease condition? Why ‘this patient’ is sick ‘this way’?
The disease diagnosis is important but in homeopathy, the cause of disease not just probed to the level of bacteria and viruses. Other factors like mental, emotional and physical stress that could predispose a person to illness also looked for. Now a days, even modern medicine also considers a large number of diseases as psychosomatic. The correct homeopathy remedy tries to correct this disease predisposition.
The focus is not on curing the disease but to cure the person who is sick, to restore the health. If a disease pathology not very advanced, homeopathy remedies do give a hope for cure but even in incurable cases, the quality of life can greatly improve with homeopathic medicines.
Homeopathic Medicines for Bipolar Disorder
The homeopathic remedies (medicines) given below indicate the therapeutic affinity but this is not a complete and definite guide to the homeopathy treatment of this condition. The symptoms listed against each homeopathic remedy may not be directly related to this disease because in homeopathy general symptoms and constitutional indications also taken into account for selecting a remedy, potency and repetition of dose by Homeopathic doctor.
So, here we describe homeopathic medicine only for reference and education purpose. Do not take medicines without consulting registered homeopathic doctor (BHMS or M.D. Homeopath).
Medicine:
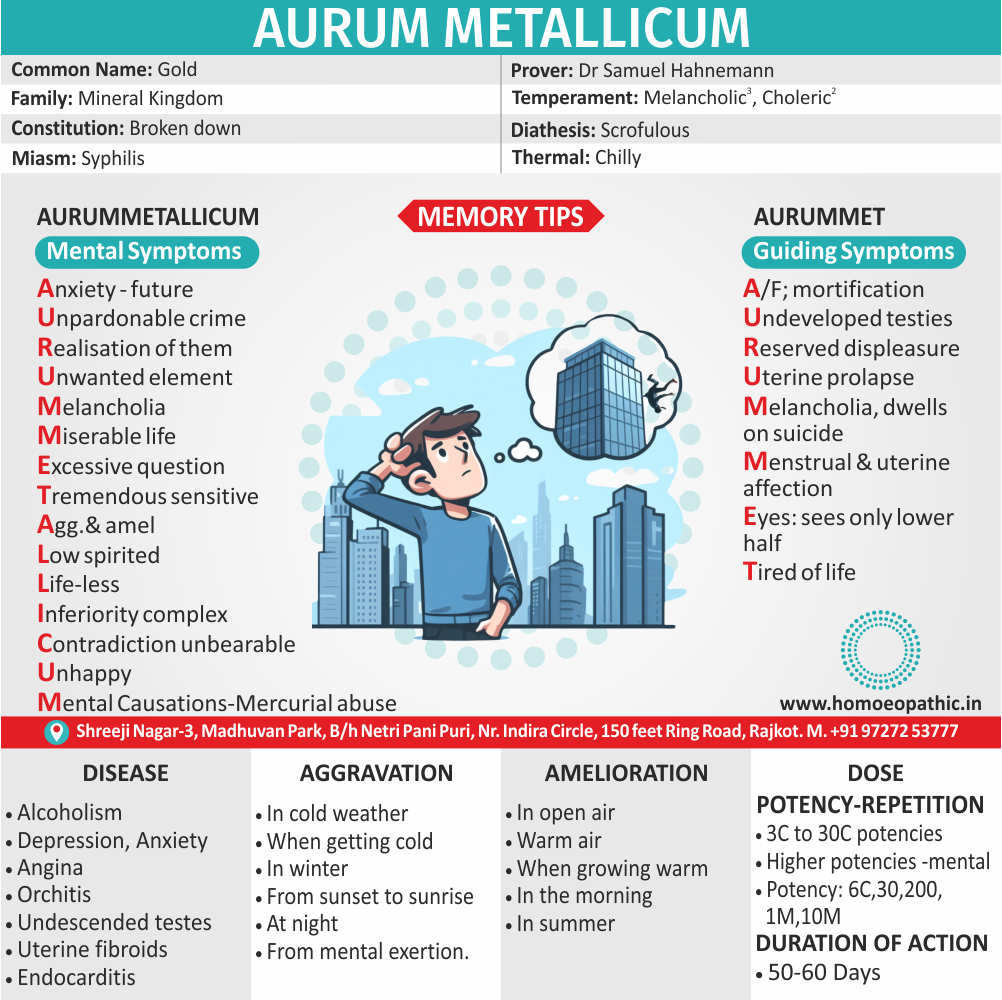
Aurum Metallicum:
It is an excellent Homeopathic medicine for treating those cases of depression in this Disorder where suicidal thoughts predominate and the patient feels hopeless and worthless and has persistent suicidal thoughts.
Natrum Sulphuricum:
It is another Homeopathic remedy of great help for a patient in whom suicidal thoughts mark and they has to apply much self-control to stop themselves from actually died by suicide. Another symptom that calls for the use of Homeopathic medicine Natrum Sulphuricum is gloominess.
When the patient of Bipolar Disorder feels sad even when listening to lively music and has an aversion to talk or spoken to, Natrum Sulphuricum is a very beneficial Homeopathic remedy.
Lilium Tigrinum
- It is of great help in treating increased energy levels in Bipolar Disorder where the main symptom is extreme restlessness and difficulty in sitting still at one place. Another feature to look out for while choosing Lilium Tigrinum is when a patient shows great hurriedness without any ambition or aim. The patient requiring this medicine usually has a heart or uterine disease associated with the mental symptoms.
Belladonna
- It works very well for those patients of Bipolar Disorder who show marked violent behavior and violence occurs in fits that come and go suddenly and the patient even bites and strikes the person near him or her. Another symptom of violence where Belladonna is beneficial as a cure is when the patient spits on people and the face turns red.
Ignatia Amara
- It is one of the best remedies for treating sadness experienced by a patient in the depressive phase of Bipolar Disorder. The patients requiring this medicine usually have a history of long-held grief like the death of a family member or close friend or in cases where the disease has originated after disappointed love affections or from suppressed emotions. Ignatia Amara is a very helpful remedy for patients who sit silently and weep or brood over the past. (3)
- Left untreated, this disorder can result in serious problems that affect every area of your life. These may include:
- Problems related to drug and alcohol use
- Suicide or suicide attempts
- Legal problems
- Financial problems
- Relationship troubles
- Isolation and loneliness
- Poor work or school performance
- Frequent absences from work or school
Diet & Regimen of Bipolar disorder:
- Eating a balance of protective, nutrient-dense foods. These foods include fresh fruits, vegetables, legumes, whole grains, lean meats, cold-water fish, eggs, low-fat dairy, soy products, and nuts and seeds.
- Avoid concentrated sources of simple sugars, such as soft drinks, fruit juices, jellies and jams, syrups, and candy bars.
- Go for Fatty Acids – Omega-3s, the essential fatty acids found in walnuts, flaxseed, and coldwater fish, such as salmon.
- Limit Alcohol and Caffeine – alcohol is a depressant.(2)
Reference:
- https://www.ncbi.nlm.nih.gov › articles › PMC2813703
- https://psychcentral.com › bipolar › bipolar-diet
- https://www.drhomeo.com/bipolar/homeopathic-remedies-for-bipolar-disorder-treatment/
Frequently Asked Questions
What is Bipolar Disorder?
Bipolar disorder ( bipolar affective disorder, manic depressive disorder) is characterized by marked mood swings between mania (mood elevation) and bipolar depression that cause significant personal distress or social dysfunction, and are not caused by drugs or known physical disorders.
Homeopathic Medicines used by Homeopathic Doctors in treatment of Bipolar Disorder?
- Aurum Metallicum
- Natrum Sulphuricum
What are the symptoms of Bipolar Disorder?
- Mood swings
- Sadness
- Elevated mood
- Anger, Anxiety, Apathy, Apprehension
- Hyperactivity, Impulsivity, Restlessness
- Unwanted thoughts, Delusion
- Lack of concentration
- Depression
- excited episode
What are the causes of Bipolar Disorder?
- Biological differences
- Imbalance in Neurotransmitters
- Inherited traits
Definition:
Bipolar disorder ( bipolar affective disorder, manic depressive disorder) is characterized by marked mood swings between mania (mood elevation) and bipolar depression that cause significant personal distress or social dysfunction, and are not caused by drugs or known physical disorders.
Overview
Epidemiology
Causes
Risk Factors
Types
Pathophysiology
Clinical Features
Sign & Symptoms
Clinical Examination
Diagnosis
Differential Diagnosis
Complications
Investigations
Treatment
Prevention
Homeopathic Treatment
Diet & Regimen
Do’s and Dont’s
Terminology
References
FAQ
Also Search As
Overview
Bipolar disorder:
This disorder, formerly called manic depression, causes extreme mood swings that include emotional highs (mania or hypomania) and lows (depression). When you become depressed, you may feel sad or hopeless and lose interest or pleasure in most activities.
When your mood shifts in the other direction, you may feel euphoric and full of energy. Mood shifts may occur only a few times a year or as often as several times a week.
Epidemiology
Indian epidemiology then other
Causes
- The exact cause of bipolar disorder is unknown, but several factors may be involved, such as:
- Biological differences. People with bipolar disorder appear to have physical changes in their brains. The significance of these changes is still uncertain but may eventually help pinpoint causes.
- Neurotransmitters. An imbalance in naturally occurring brain chemicals called neurotransmitters seems to play a significant role in this disorder and other mood disorders.
- Inherited traits. Bipolar disorder is more common in people who have a first-degree relative, such as a sibling or parent, with the condition. Researchers are trying to find genes that may be involved in causing bipolar disorder.
Risk Factors
- Factors that may increase the risk of developing this disorder or act as a trigger for the first episode include:
- Having a first-degree relative, such as a parent or sibling, with bipolar disorder
- Periods of high stress
- Either Drug or alcohol abuse
- Major life changes, such as the death of a loved one or other traumatic experiences
Types
Types of Bipolar disorder
- Bipolar I disorder- involves periods of severe mood episodes from mania to depression.
- Bipolar II disorder- is a milder form of mood elevation, involving milder episodes of hypomania that alternate with periods of severe depression.
- Cyclothymic disorder- describes brief periods of hypomanic symptoms alternating with brief periods of depressive symptoms that are not as extensive or as long-lasting as seen in full hypomanic episodes or full depressive episodes.
- "Mixed features" – refers to the occurrence of simultaneous symptoms of opposite mood polarities during manic, hypomanic or depressive episodes. It’s marked by high energy, sleeplessness, and racing thoughts. At the same time, the person may experience hopeless, despairing, irritable, and suicidal feelings.
Rapid-cycling- is a term that describes having four or more mood episodes within a 12-month period. Episodes must last for some minimum number of days in order to be considered distinct episodes. Some people also experience changes in polarity from high to low or vice-versa within a single week, or even within a single day, meaning that the full symptom profile that defines distinct, separate episodes may not be present (for example, the person may not have a decreased need for sleep). Sometimes called "ultra-rapid" cycling, there is debate within psychiatry as to whether this phenomenon is a valid or well-established feature in bipolar disorder. A pattern of rapid cycling can occur at any time in the course of illness, although some researchers believe that it may be more common at later points in the lifetime duration of illness. Women appear more likely than men to have rapid cycling. A rapid-cycling pattern increases risk for severe depression and suicide attempts. Antidepressants may sometimes be associated with triggering or prolonging periods of rapid cycling. However, that theory is controversial and is still being studied. (2)
Pathophysiology
Pathophysiology of Bipolar disorder
- It is characterized by dysregulation in the dopamine and serotonin systems and by pathology in the brain systems involved in regulating emotion.
- Psychosocial stressors, notably life events and familial expressed emotion, significantly influence the course of the illness in the context of these vulnerabilities.
Clinical Features
Tab Content
Sign & Symptoms
Mania:
Mania, a syndrome which is in some ways the reverse of depression, occurs as part of bipolar disorder. The term bipolar disorder implies episodes of both mania and depressive disorder, but the diagnostic category also includes those who, at the time of diagnosis, have suffered
only manic illnesses (most patients with mania eventually develop a depressive disorder). When manic symptoms occur without significant psychosocial impairment,
the syndrome is called hypomania.
The features of mania are;
- elevated mood,
- overactivity,
- and poor judgement.
Mania occurs as part of bipolar disorder in which there may also episodes of depression.
Mania is considerably less common than depressive disorder; it is important that mania recognize in its early stages because in the later stages the patient becomes increasingly unwilling to accept treatment. Long-term maintenance drug treatment to prevent relapse should considere in the management of patients with recurrent bipolar illnesses.
Clinical Examination
Clinical examination:
Bipolar disorder is characterized by periods depression that alternate with periods of mania. Physical examination of patients with bipolar disorder is usually normal. A mental status examination physical examination should assess patients for
Major depression for 2 weeks being either a depressed mood or loss of pleasure, and presence of at least five of the following symptoms:
- Depressed mood
- Markedly diminished interest in nearly all activities
- marked weight loss or gain or significant loss or increase in appetite
- Hypersomnia or insomnia
- Psychomotor retardation or agitation
- Loss of energy or fatigue
- Feelings of worthlessness or excessive guilt
- Decreased concentration ability
- Preoccupation with death or suicide.
Mania: feature at least 1 week of profound mood disturbance, characterized by elation, irritability, or expansiveness and at least 3 of the diagnostic criteria
- Grandiosity
- Diminished need for sleep
- Excessive talking
- Racing thoughts
- Clear evidence of distractibility
- Increased level of goal-focused activity at home, at work.
- Excessive pleasurable activities.
- Hypomania characterized by an elevated, or irritable mood of at least 4 consecutive days duration. for diagnosis it require at least three of the symptoms of mania.
- Impulsive or risk-taking behaviors
- Suicidal thoughts and behavior
- Risk factors for suicide attempts and deaths.
- In addition to current symptoms, it is important to ascertain the number, frequency, intensity, and duration of past mood episodes.
Examination using the Mental Status Examination as well as assessment of the following:
- Appearance
- Affect/mood
- Thought content
- Perception
- Suicide/self-destruction
- Homicide/violence/aggression
- Judgment/insight
- Cognition
- Physical health
Diagnosis
Diagnostic criteria for bipolar and related disorders are based on the specific type of disorder:
- Bipolar I disorder: You’ve had at least one manic episode. The manic episode may be preceded by or followed by hypomanic or major depressive episodes. Mania symptoms cause significant impairment in your life and may require hospitalization or trigger a break from reality (psychosis).
- Bipolar II disorder: You’ve had at least one major depressive episode lasting at least two weeks and at least one hypomanic episode lasting at least four days, but you’ve never had a manic episode. Major depressive episodes or the unpredictable changes in mood and behavior can cause distress or difficulty in areas of your life.
- Cyclothymic disorder: You’ve had at least two years — or one year in children and teenagers — of numerous periods of hypomania symptoms (less severe than a hypomanic episode) and periods of depressive symptoms (less severe than a major depressive episode). During that time, symptoms occur at least half the time and never go away for more than two months. Symptoms cause significant distress in important areas of your life.
Criteria for a manic or hypomanic episode:
The DSM-5 has specific criteria for the diagnosis of excited and hypomanic episodes i.e.:
- Firstly, A manic episode is a distinct period of abnormally and persistently elevated, expansive or irritable mood that lasts at least one week (or less than a week if hospitalization is necessary). The episode includes persistently increased goal-directed activity or energy.
- Secondly, A hypomanic episode is a distinct period of abnormally and persistently elevated, expansive or irritable mood that lasts at least four consecutive days.
Criteria for a major depressive episode:
- The DSM-5 also lists criteria for diagnosis of a major depressive episode:
- Five or more of the symptoms below over a two-week period that represent a change from previous mood and functioning. At least one of the symptoms is either depressed mood or loss of interest or pleasure.
- Symptoms can be based on your own feelings or on the observations of someone else.
Differential Diagnosis
Differential diagnosis of Bipolar disorder
- Major depressive disorder
- Cyclothymic disorder
- Psychotic disorders
- Anxiety disorders
- ADHD
- Personality disorders (4)
Conditions that commonly occur with bipolar disorder:
If you have this disorder, you may also have another health condition that’s diagnosed before or after your diagnosis of bipolar disorder.
Such conditions need to diagnose and treat because they may worse existing bipolar disorder or make treatment less successful. They i.e.:
- Anxiety disorders: For Examples include social anxiety disorder and generalized anxiety disorder.
- Post-traumatic stress disorder (PTSD): Some people with PTSD, a trauma- and stressor-related disorder, also have this disorder.
- Attention-deficit/hyperactivity disorder (ADHD): ADHD has symptoms that overlap with this disorder. For this reason, this disorder can be difficult to differentiate from ADHD. Sometimes one is mistaken for the other. In some cases, a person may be diagnosed with both conditions.
- Addiction or substance abuse: Many people with maniac disorder also have alcohol, tobacco or drug problems. Drugs or alcohol may seem to ease symptoms, but they can actually trigger, prolong or worsen depression or mania.
- Physical health problems: People diagnosed with this disorder are more likely to have certain other health problems, such as heart disease, thyroid problems or obesity.
Complications
- Left untreated, this disorder can result in serious problems that affect every area of your life. These may include:
- Problems related to drug and alcohol use
- Suicide or suicide attempts
- Legal problems
- Financial problems
- Relationship troubles
- Isolation and loneliness
- Poor work or school performance
- Frequent absences from work or school
Investigations
Investigation of Bipolar disorder
- There are no specific blood tests or brain scans to diagnose bipolar disorder.
- May perform a physical exam and order lab tests, including a thyroid function test and urine analyses.
Treatment
Treatment of Bipolar disorder
- Psychotherapy
- Social Rhythm Therapy
- Cognitive Behavioral Therapy
- Electroconvulsive therapy
- Do regular physical exercise
- Drug Treatment
Prevention
Tab Content
Homeopathic Treatment
Homeopathic Treatment of Bipolar Disorder
Homeopathy treats the person as a whole. It means that homeopathic treatment focuses on the patient as a person, as well as his pathological condition. The homeopathic medicines selected after a full individualizing examination and case-analysis.
Which includes
- The medical history of the patient,
- Physical and mental constitution,
- Family history,
- Presenting symptoms,
- Underlying pathology,
- Possible causative factors etc.
A miasmatic tendency (predisposition/susceptibility) also often taken into account for the treatment of chronic conditions.
What Homoeopathic doctors do?
A homeopathy doctor tries to treat more than just the presenting symptoms. The focus is usually on what caused the disease condition? Why ‘this patient’ is sick ‘this way’?
The disease diagnosis is important but in homeopathy, the cause of disease not just probed to the level of bacteria and viruses. Other factors like mental, emotional and physical stress that could predispose a person to illness also looked for. Now a days, even modern medicine also considers a large number of diseases as psychosomatic. The correct homeopathy remedy tries to correct this disease predisposition.
The focus is not on curing the disease but to cure the person who is sick, to restore the health. If a disease pathology not very advanced, homeopathy remedies do give a hope for cure but even in incurable cases, the quality of life can greatly improve with homeopathic medicines.
Homeopathic Medicines for Bipolar Disorder
The homeopathic remedies (medicines) given below indicate the therapeutic affinity but this is not a complete and definite guide to the homeopathy treatment of this condition. The symptoms listed against each homeopathic remedy may not be directly related to this disease because in homeopathy general symptoms and constitutional indications also taken into account for selecting a remedy, potency and repetition of dose by Homeopathic doctor.
So, here we describe homeopathic medicine only for reference and education purpose. Do not take medicines without consulting registered homeopathic doctor (BHMS or M.D. Homeopath).
Medicine:
Aurum Metallicum:
It is an excellent Homeopathic medicine for treating those cases of depression in this Disorder where suicidal thoughts predominate and the patient feels hopeless and worthless and has persistent suicidal thoughts.
Natrum Sulphuricum:
It is another Homeopathic remedy of great help for a patient in whom suicidal thoughts mark and they has to apply much self-control to stop themselves from actually died by suicide. Another symptom that calls for the use of Homeopathic medicine Natrum Sulphuricum is gloominess.
When the patient of Bipolar Disorder feels sad even when listening to lively music and has an aversion to talk or spoken to, Natrum Sulphuricum is a very beneficial Homeopathic remedy.
Lilium Tigrinum
- It is of great help in treating increased energy levels in Bipolar Disorder where the main symptom is extreme restlessness and difficulty in sitting still at one place. Another feature to look out for while choosing Lilium Tigrinum is when a patient shows great hurriedness without any ambition or aim. The patient requiring this medicine usually has a heart or uterine disease associated with the mental symptoms.
Belladonna
- It works very well for those patients of Bipolar Disorder who show marked violent behavior and violence occurs in fits that come and go suddenly and the patient even bites and strikes the person near him or her. Another symptom of violence where Belladonna is beneficial as a cure is when the patient spits on people and the face turns red.
Ignatia Amara
- It is one of the best remedies for treating sadness experienced by a patient in the depressive phase of Bipolar Disorder. The patients requiring this medicine usually have a history of long-held grief like the death of a family member or close friend or in cases where the disease has originated after disappointed love affections or from suppressed emotions. Ignatia Amara is a very helpful remedy for patients who sit silently and weep or brood over the past. (3)
Diet & Regimen
Diet & Regimen of Bipolar disorder:
- Eating a balance of protective, nutrient-dense foods. These foods include fresh fruits, vegetables, legumes, whole grains, lean meats, cold-water fish, eggs, low-fat dairy, soy products, and nuts and seeds.
- Avoid concentrated sources of simple sugars, such as soft drinks, fruit juices, jellies and jams, syrups, and candy bars.
- Go for Fatty Acids – Omega-3s, the essential fatty acids found in walnuts, flaxseed, and coldwater fish, such as salmon.
- Limit Alcohol and Caffeine – alcohol is a depressant.(2)
Do’s and Dont’s
Tab Content
Terminology
Tab Content
References
Reference:
- https://www.ncbi.nlm.nih.gov › articles › PMC2813703
- https://psychcentral.com › bipolar › bipolar-diet
- https://www.drhomeo.com/bipolar/homeopathic-remedies-for-bipolar-disorder-treatment/
FAQ
Frequently Asked Questions
What is Bipolar Disorder?
Bipolar disorder ( bipolar affective disorder, manic depressive disorder) is characterized by marked mood swings between mania (mood elevation) and bipolar depression that cause significant personal distress or social dysfunction, and are not caused by drugs or known physical disorders.
Homeopathic Medicines used by Homeopathic Doctors in treatment of Bipolar Disorder?
- Aurum Metallicum
- Natrum Sulphuricum
What are the symptoms of Bipolar Disorder?
- Mood swings
- Sadness
- Elevated mood
- Anger, Anxiety, Apathy, Apprehension
- Hyperactivity, Impulsivity, Restlessness
- Unwanted thoughts, Delusion
- Lack of concentration
- Depression
- excited episode
What are the causes of Bipolar Disorder?
- Biological differences
- Imbalance in Neurotransmitters
- Inherited traits
Also Search As
Frequently Asked Questions (FAQ)
XYZ
XXX
XYZ
XXX
XYZ
XXX
People found Homeopathic Clinic For XXXX by searching for
XXX
People found Homeopathic Doctors for XXXX by searching for
XXX
People found Homeopathic treatment for XXXX by searching for
XXX