Definition:
There is a commonly held view that eating disorders are a lifestyle choice. Eating disorders are actually serious and often fatal illnesses that cause severe disturbances to a person’s eating behaviors. Obsessions with food, body weight, and shape may also signal an eating disorder.
Overview
Epidemiology xxx
Causes
Types
Risk Factors
Pathogenesis xxx
Pathophysiology xxx
Clinical Features xxx
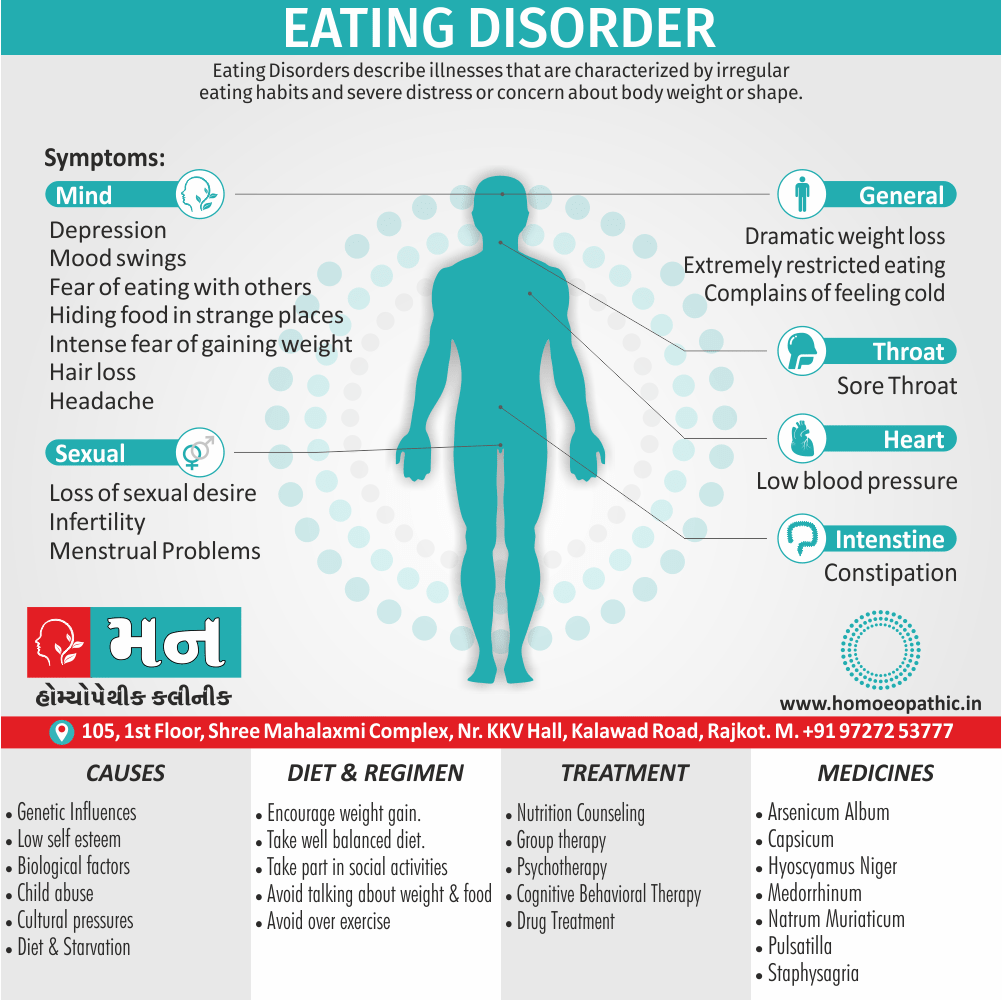
Sign & Symptoms
Clinical Examination
Diagnosis
Differential Diagnosis
Complications xxx
Investigations
Treatment
Prevention
Homeopathic Treatment
Diet & Regimen
Do’s and Dont’s xxx
Terminology xxx
References
FAQ
Also Search As xxx
Overview
Overview of Eating Disorder
Obsessions with food, body weight, and shape may also signal an eating disorder.
The two specific diagnosis noted in the DSM-IV include anorexia nervosa, bulimia nervosa, and binge-eating disorder i.e.:
- Anorexia Nervosa
- Bulimia Nervosa
- Compulsive Overeating or Binge Eating Disorder
- Obesity (in other words, Overeating Associated with Other Psychological Disturbances)
- Psychogenic Vomiting
Epidemiology xxx
Indian epidemiology then other
Causes
Cause of Eating Disorder
The exact cause of eating disorders is unknown. As with other mental illnesses, there may be many causes, such as:
- Genetics and biology: Certain people may have genes that increase their risk of developing eating disorders. Biological factors, such as changes in brain chemicals, may play a role in eating disorders.
- Psychological and emotional health: People with eating disorders may have psychological and emotional problems that contribute to the disorder. They may have low self-esteem, perfectionism, impulsive behavior and troubled relationships.
- Biological factors
- Child abuse
- Cultural pressures
- Diet & Starvation (3)
Types
Types of Eating Disorder
The two specific diagnosis noted in the DSM-IV include anorexia nervosa, bulimia nervosa, and binge-eating disorder.
1. Anorexia nervosa:
Generally, This Eating Disorder is characterized by refusal to maintain a minimally normal body weight.
Prominent clinical features:
It occurs much more often in females as compared to the males. In detail, The common age of onset is adolescence (13-19 years of age). [1]
There is an intense fear of becoming obese. Additionally, This fear does not decrease even if body becomes very thin and underweight. [1]
The Eating Disorder, Anorexia, is a unique reaction to a variety of external and internal conflicts, such as stress, anxiety, unhappiness also feeling like life is out of control. [2]
There is often a body-image disturbance. The person is unable to perceive own body size accurately. [1]
New research indicates that for a percentage of sufferers, a genetic predisposition may play a role in a sensitivity to develop Besides this, Anorexia, with environmental factors being the trigger. [2]
People with anorexia nervosa typically weigh themselves repeatedly, severely restrict the amount of food they eat, and eat very small quantities of only certain foods. Lastly, They may be afraid of losing control over the amount of food they eat, accompanied by the desire to control their emotions and reactions to their emotions. [2]
Mortality rate
Anorexia nervosa has the highest mortality rate of any mental disorder. While many young women and men with this disorder die from complications associated with starvation, others die of suicide. In women, suicide is much more common in those with anorexia than with most other mental disorders.
With a low self-esteem and need for acceptance they will turn to obsessive dieting and starvation as a way to control not only their weight, but their feelings also actions regarding; the emotions attached. [2]
Some also feel that they do not deserve pleasure out of life, and will deprive themselves of situations offering pleasure (including eating). [2]
Amenorrhoea, primary or secondary, is often present in females. Women with anorexia nervosa can present with poor sexual adjustment, with conflicts about being a woman and fear of pregnancy. [1]
Behavioral signs
Some of the behavioural signs can be: obsessive exercise, calorie and fat gram counting, starvation and restriction of food, self-induced vomiting, the use of diet pills, laxatives or diuretics to attempt controlling weight, and a persistent concern with body image. [2]
If untreated, the weight loss can become marked. Death may occur due to hypokalemia (caused by self-induced vomiting), dehydration, malnutrition or congestive cardiac failure (caused by anaemia). [1]
Symptoms include:
- Extremely restricted eating
- Extreme thinness (in other words, emaciation)
- A relentless pursuit of thinness and unwillingness to maintain a normal or healthy weight
- Intense fear of gaining weight.
- Distorted body image, a self-esteem that is heavily influenced by perceptions of body weight and shape, or a denial of the seriousness of low body weight.
2. Bulimia nervosa:
It is characterized by recurrent and frequent episodes of eating unusually large amounts of food and feeling a lack of control over these episodes. This binge-eating is followed by behavior that compensates for the overeating such as forced vomiting, excessive use of laxatives or diuretics, fasting, excessive exercise, or a combination of these behaviors. [2]
There is an intense fear of becoming obese. There may be an earlier history of anorexia nervosa.
It is usually body-image disturbance and the person is unable to perceive own body size accurately. [1]
There is a persistent preoccupation with eating, and an irresistible craving for food. There are episodes of overeating in which large amounts of food are consumed within short periods of time (in other words, eating binges). [1]
This can be indirect relation to how they feel about themselves, or how they feel over a particular event or series of events in their lives. [2]
Reasearch
New research indicates that for a percentage of sufferers, a genetic predisposition may play a role in a sensitivity to develop Bulimia, with environmental factors being the trigger. [2]
Men and women suffering Bulimia are usually aware they have an eating disorder. [2]
Fascinated by food they sometimes buy magazines and cookbooks to read recipes, and enjoy discussing dieting issues. [2]
Some of the behavioural signs can be: Recurring episodes of rapid food consumption followed by tremendous guilt and purging (i.e. laxatives or self-induced vomiting), a feeling of lacking control over his or her eating behaviours, regularly engaging in stringent diet plans and exercise, the misuse of laxatives, diuretics, and/or diet pills and a persistent concern with body image can all be warning signs someone is suffering with Bulimia. [2]
Symptoms i.e.:
- Chronically inflamed and sore throat
- Swollen salivary glands in the neck and jaw area
- Worn tooth enamel and increasingly sensitive and decaying teeth as a result of exposure to stomach acid
- Acid reflux disorder and other gastrointestinal problems
- Intestinal distress and irritation from laxative abuse
- Severe dehydration from purging of fluids
- Electrolyte imbalance (too low or too high levels of sodium, calcium, potassium and other minerals) which can lead to stroke or heart attack.
3. Compulsive Overeating or Binge Eating disorder :
Binge-eating disorder is the most common eating disorder in the U.S. People with binge-eating disorder lose control over his or her eating. Unlike bulimia nervosa, periods of binge-eating are not followed by purging, excessive exercise, or fasting.
As a result, people with binge-eating disorder often are overweight or obese. [1]
Additionally, there also may be eating of large amounts of food throughout the day with no planned meal times, eating alone because of being embarrassed, and/or feeling guilty and depressed after overeating. [1]
The disorder is not listed separately in ICD-10 and symptoms of binge eating are also seen in bulimia nervosa. [1]
Fear of not being able to control eating, also while eating, not being able to stop. [2]
Isolation. Fear of eating around and with others. [2]
Chronic dieting on a variety of popular diet plans. [2]
Holding the belief that life will be better if they can lose weight. [2]
Symptoms include:
- Eating unusually large amounts of food in a specific amount of time
- Eating until you are uncomfortably full.
- Feeling distressed, ashamed, or guilty about your eating.
- Frequently dieting, possibly without weight loss.
- Hiding food in strange places ( e.g. closets, cabinets, suitcases, under the bed) to eat at a later time. Either Vague or secretive eating patterns. [2]
- Self-defeating statements after food consumption. [2]
- Eating even when you’re full or not hungry.
- Eating fast during binge episodes.
- Blames failure in social and professional community on weight. [2]
- Holding the belief that food is their only friend. [2]
Other symptoms
- Frequently out of breath after relatively light activities. [2]
- Excessive sweating also shortness of breath. [2]
- High blood pressure also cholesterol. [2]
- Eating alone or in secret to avoid embarrassment.
- Leg and joint pain. [2]
- Weight gain. [2]
- Decreased mobility due to weight gain. [2]
- Loss of either sexual desire or promiscuous relations. [2]
- Mood swings, depression, fatigue. [2]
- Insomnia, poor sleeping habits. [2]
4. Obesity (Overeating Associated with Other Psychological Disturbances):
Obesity caused by a reaction to distressing events is included here. It caused by drugs or endocrine factors, or due to constitutional factors is not considered a psychiatric disorder. [1]
5. Psychogenic Vomiting:
This is clinical syndrome in which biopsychosocial factors interact to produce symptoms which are often mistaken for upper gastrointestinal tract disease, anorexia nervosa, dissociative (conversion) disorder, somatization disorder, or malingering.
The characteristic clinical features include:
- Repeated vomiting, which typically occurs soon after a meal has begun or just after it has been completed.
- Vomiting often occurs in complete absence of nausea or retching (Patients say that food just seems to come back up).
- Vomiting is often self-induced and can be suppressed, if necessary.
- Despite repeated vomiting, weight loss is not usually significant.
- The course of illness is usually chronic with frequent remissions and relapses.
Risk Factors
Risk factors of eating disorder
- Eating disorders frequently appear during the teen years or young adulthood but may also develop during childhood or later in life.
- These disorders affect both genders, although rates among women are 2½ times greater than among men.
- Like women who have eating disorders, men also have a distorted sense of body image.
- For example, men may have muscle dysmorphia, a type of disorder marked by an extreme concern with becoming more muscular.
Pathogenesis xxx
Tab Content
Pathophysiology xxx
Tab Content
Clinical Features xxx
Tab Content
Sign & Symptoms
Sign & Symptoms of Eating Disorder
- Dramatic weight loss in a relatively short period of time.
- Wearing big or baggy clothes or dressing in layers to hide body shape also weight loss.
- Furthermore, Obsession with weight and complaining of weight problems ( even if "average" weight or thin).
- Additionally, Obsession with continuous exercise.
- Besides this, Frequent trips to the bathroom immediately following meals (occasionally, accompanied with water running in the bathroom for a long period of time to hide the sound of vomiting).
- In brief, Visible food restriction and self-starvation.
- Visible bingeing also purging.
- All in all, Use or hiding use of diet pills, laxatives, ipecac syrup ( can cause immediate death !) or enemas.
Isolation
- Fear of eating around and with others.
Unusual food rituals such as shifting the food around on the plate to look eaten; cutting food into tiny pieces; additionally, making sure the fork avoids contact with the lips (using teeth to scrap food off the fork or spoon); chewing food also spitting it out, but not swallowing; dropping food into napkin on lap to later throw away.
Obsession with calories also fat content of foods.
Hiding food in strange places (e.g. closets, cabinets, suitcases, under the bed) to avoid eating (in other words, Anorexia) or to eat at a later time (in other words, Bulimia).
Moreover, Flushing uneaten food down the toilet (can cause sewage problems).
Vague or secretive eating patterns.
Lastly, Keeping a "food diary" or lists that consists of food also behaviours (i.e., purging, restricting, calories consumed, exercise, etc.)
Other symptoms
- Preoccupied thoughts of food, weight also cooking.
- Visiting websites, which promote unhealthy ways to lose weight.
- Additionally, Reading books about weight loss and eating disorders.
- Self-defeating statements after food consumption.
- Hair loss. Either Pale or "gray" appearance to the skin.
- Dizziness also headaches.
- Frequent sore throats also swollen glands.
- In detail, Low self-esteem. Feeling worthless. Often putting themselves down · also complaining of being "too stupid" or "too fat" and saying they do not matter. Need for acceptance and approval from others.
- Complaints of often feeling cold.
- Low blood pressure.
- Moreover, Loss of menstrual cycle.
- Constipation or incontinence.
- Either Bruised or calluses knuckles; bloodshot or bleeding in the eyes; light bruising under the eyes also on the cheeks.
- Perfectionist personality.
- Loss of sexual desire or promiscuous relations.
- Mood swings, depression, fatigue.
- Insomnia. All in all, Poor sleeping habits.
Clinical Examination
Clinical examination of eating disorder
The Eating Disorder Examination assesses the frequency of disordered eating behaviors over the past 28 days. The questions are organized into four groupings: restraint, eating concern, shape concern, and weight concern.
Four groupings of the EDE
The portion of the Eating Disorder Examination concerned with restraint asks questions about restraint overeating, avoiding specific foods, dietary rules, avoidance of eating, and emptiness felt in the stomach.
The eating concern portion of the Eating Disorder Examination asks about preoccupation with food, fear of losing control overeating, eating in secret, social eating, and guilt after eating.
The shape concern portion of the Eating Disorder Examination asks about body concerns including specifically a flat stomach, preoccupation with body shape or weight, the importance of shape, fear of weight gain, dissatisfaction with body shape, discomfort in seeing the body, avoidance of exposure of the body, and feelings of fatness.
The weight concern portion of the Eating Disorder Examination investigates the importance of weight to the patient, any reactions to prescribed weighing, preoccupation with body shape and weight, dissatisfaction with current weight, and a desire to lose weight.
The Eating Disorder Examination tool is extensive and may be part of a larger medical examination for determining if a patient has an eating disorder. The full medical examination for an eating disorder may also include a medical history, a physical exam, and various clinical or diagnostic tests. (4)
Diagnosis
Diagnosis of Eating Disorder
- Researchers are finding that eating disorders are caused by a complex interaction of genetic, biological, behavioral, psychological, and social factors.
- Eating disorders run in families. Researchers are working to identify DNA variations that are linked to the increased risk of developing eating disorders.
- Brain imaging studies are also providing a better understanding of eating disorders.
- For example, researchers have found differences in patterns of brain activity in women with eating disorders in comparison with healthy women.
Differential Diagnosis
Differential diagnosis of eating disorder
- Anxiety
- Depression
- Obsessive-compulsive disorder (OCD)
- Post-traumatic stress disorder (PTSD)
- Addiction like Laxatives, Diuretics, Diet pills
- Diabulimia
- Pregnancy (5)
Complications xxx
Complications are what happen after you have a disease. They are the negative consequences of the disease process.
Investigations
Investigation of Eating Disorder
While there is no one specific lab test to confirm an eating disorder diagnosis.
Your healthcare provider will likely want a blood test to check your complete blood count (CBC), along with your:
- Electrolytes
- Liver function
- Kidney function
- Thyroid function
- X-Ray
- ECG (5)
Treatment
Treatment of Eating Disorder
Treatment of anorexia nervosa:
It can be considered in two phases, which often merge into each other.
- Short-term treatment: to encourage weight gain and correct nutritional deficiencies, if any.
- Long-term treatment: aimed at maintaining the near normal weight achieved in short-term treatment and preventing relapses. [1]
1. Behaviour therapy (BT):
Behavioural treatments are based on providing positive reinforcements (and at times, negative reinforcements) contingent on weight gain by the patient.The weight gain should not exceed 1.5 to 2 kg in a fortnight. As patients are usually unable to eat a large meal, especially in the initial part of treatment, it is advisable to suggest more number of meals (about six) per day.
Occasionally, forceful Ryle’s tube feeding may be needed initially, in resistant patients. [1]
2. Individual psychotherapy:
It is often helpful in addition to supportive physical treatment. This could involve psychotherapy with a focus on cognitive behaviour therapy, psychodynamic principles or supportive measures. [1]
3. Hospitalisation:
Hospitalisation with adequate nursing care for food intake and weight gain, can be helpful in short-term treatment as well as prevention and/ or treatment of complications. It is important to keep a close eye on water and electrolyte balance, need for supplementation with vitamins and minerals, also prevent osteoporosis. [1]
4. Drugs:
i. Antipsychotics:
Chlorpromazine is rarely used these days. Furthermore, Olanzapine has efficacy in improving weight gain but it is important to be aware of possibility of prolongation of QTc particularly in patients with low BMI.
ii. Antidepressants:
(e.g. fluoxetine, clomipramine) for treatment of anorexia nervosa and/ or associated depression.
iii. Cyproheptadine:
In brief, This is particularly helpful in inducing weight gain, decreasing depressive symptoms also increasing appetite, if anorexia is actually present. The usual dose is 8-32 mg/ day, in divided doses.
5. Group therapy and family therapy:
It can be helpful in psycho-education for the patient and carers/ family about nature of anorexia nervosa and its treatment. Psycho-education may also include discussion of current social norms of slimming and fitness. [1]
Treatment of Bulimia Nervosa and Binge Eating disorder:
1. Behaviour therapy:
This is based on providing positive reinforcements (also at times negative reinforcements) contingent on the control of binge eating by the patient. [1]
2. Individual psychotherapy.
3. Antidepressant drugs:
They are an important adjunct to other modes of therapy.
A Selective serotonin uptake inhibitor (in other words, SSRI) such as Fluoxetine (in doses of 20-60 mg) is particularly useful as it can cause loss of appetite at least in the initial phase of treatment, along with its antidepressant effect.
The drugs used in the past have included tricyclic antidepressants such as imipramine, though they are currently not widely used. [1]
4. Group therapy and family therapy:
These methods are used for psycho-education of patient and carers/family about nature of bulimia nervosa and its treatment. [1]
Treatment of Obesity (Overeating Associated with Other Psychological Disturbances):
It depend on the underlying cause; for example, psychotherapy (for present or past psychological distress), antidepressants (for depression), advice from dietician, drug treatment, or even bariatric surgery. [1]
Treatment of psychogenic vomiting:
1. The first and most important step is correct diagnosis and exclusion of other physical and/or psychiatric causes.
2. Identification of psychosocial stressor.
3. Environmental manipulation and encouragement of coping strategies to deal with stress.
4. Psychotherapy of either cognitive behavioural or psychodynamic nature. [1]
Prevention
Prevention of Eating Disorder
- Set a good example by eating well- If you live with or know someone who might be at risk for developing an eating disorder, you can help them by being a good role model. Eat regular, nutritious meals and choose healthy snacks when you get hungry between mealtimes
- Encourage your loved one to eat when they are hungry- Talk to them about how to listen to their body and recognize the signals that they are hungry or full. Discuss how being mindful when eating can help them meet their body’s needs and avoid over- or undereating.
- Avoid making negative or shaming comments about food and eating- Help your loved ones maintain a healthy relationship with food and eating by focusing on the positive. Don’t make critical or judgmental comments about what others are eating, and also avoid talking negatively about your own eating habits.
- Keep healthy foods around the house- If you’re concerned about the eating habits of someone you live with, make sure they have access to plenty of fresh, nutritious foods. Keep your fridge and cabinets stocked with lots of fruits, vegetables, and healthy snack options, such as yoghurt, nuts, or whole wheat crackers.
- Educate yourself and your family about how diet can affect your health- Take some time to learn about the benefits of eating healthy and the potential consequences of not eating well. Check out some books on nutrition from your library or get some information from your family doctor or a registered dietitian. Talk with your family about issues like.
- Practice positive talk about people’s bodies.
- Discuss healthy ways to cope with stress and negative feelings.(6)
Homeopathic Treatment
Homoeopathic Treatment:
Homeopathic Treatment of Eating Disorder
Homeopathy treats the person as a whole. It means that homeopathic treatment focuses on the patient as a person, as well as his pathological condition. The homeopathic medicines selected after a full individualizing examination and case-analysis.
Which includes
- The medical history of the patient,
- Physical and mental constitution,
- Family history,
- Presenting symptoms,
- Underlying pathology,
- Possible causative factors etc.
A miasmatic tendency (predisposition/susceptibility) also often taken into account for the treatment of chronic conditions.
What Homoeopathic doctors do?
A homeopathy doctor tries to treat more than just the presenting symptoms. The focus is usually on what caused the disease condition? Why ‘this patient’ is sick ‘this way’?
The disease diagnosis is important but in homeopathy, the cause of disease not just probed to the level of bacteria and viruses. Other factors like mental, emotional and physical stress that could predispose a person to illness also looked for. Now a days, even modern medicine also considers a large number of diseases as psychosomatic. The correct homeopathy remedy tries to correct this disease predisposition.
The focus is not on curing the disease but to cure the person who is sick, to restore the health. If a disease pathology not very advanced, homeopathy remedies do give a hope for cure but even in incurable cases, the quality of life can greatly improve with homeopathic medicines.
Homeopathic Medicines for Eating Disorder:
The homeopathic remedies (medicines) given below indicate the therapeutic affinity but this is not a complete and definite guide to the homeopathy treatment of this condition. The symptoms listed against each homeopathic remedy may not be directly related to this disease because in homeopathy general symptoms and constitutional indications also taken into account for selecting a remedy, potency and repetition of dose by Homeopathic doctor.
So, here we describe homeopathic medicine only for reference and education purpose. Do not take medicines without consulting registered homeopathic doctor (BHMS or M.D. Homeopath).
Anorexia Remedies: [2]
Arsenicum alb:
Extreme fastidiousness especially about germs and dirt. Anorexia coupled with fear of being poisoned. Fear of getting certain diseases so they start starving.
Carcinosin:
Obsessive compulsive disorder. Perfectionism, fear of becoming fat, fear of rejection. Etiology-abuse, grief or fears, often related to weight. Chronic insomnia, workaholics.
Hyoscyamus:
Anorexia plus mania, insanity, fear of being poisoned. Could have pathological jealousy, over concern about weight and getting fat.
Ignatia:
Perfectionism, fear of becoming fat, fear of rejection. Hysteria loss of control of emotions, fainting. Etiology-grief or big disappointment, often related to weight.
Natrum mur:
Most often indicated remedy in anorexia, a lot of guilt. Fear of being rejected, hurt easily, very self-conscious. Dry lips, emaciate, and dry skin, constipated, lose appetite. Behind this is perfectionism and fear of becoming fat. Nat mur have more confidence.
Phosphoric acid:
Etiology-grief with loss of appetite with emaciation, pining away from loss of love, second stage they get indifferent to all emotions and food. Deadness inside (Sepia, Aurum met). Grief anorexia than some chronic disease.
Platina met:
Obsessed with their appearance, fear of becoming fat. Very obsessive and impulsive personality, egocentric and arrogant, all tied up with their sexuality, religious mania.
Pulsatilla:
Feeling of worthlessness, unloved, loneliness, fixed ideas about. Food especially certain foods are bad, than amount of foods that are bad grows, fear of gaining weight, pulsatilla gain weight easily, they can eat a pastry and swear they gained weight. Ignatia, Puls. and Nat. mur. Are constantly weighing themselves. Scanty menses.
Sepia:
Anorexia plus hormonal problems, nausea, sensitivity to smell. Disgust for food, worse since childbirth, hormones causes lack of appetite.
Staphysagria:
Acute of Carcinosin, more visible, visibly upset. Carcinosin can control it more, Staph. may it more. Additionally, Deep sense of worthlessness and depression, even suicidal. Humiliation, mortified, put down, criticized, zero confidence. Fear of becoming fat and neglected by others.
Tarentula:
Mania could be religious mania. In detail, Underneath you have a fear of being poisoned. Obsessiveness about weight, very restless and hyper energy people, they do everything fast-talk, move.
Thuja occid:
In brief, Fear of being impure, dirty blood, anxiety about health, obsessed with idea of have to clean them out. Fear of eating more also becoming fat.
Veratrum alb:
Religious mania, loquacious, end of world is coming. Punish themselves, fast to appease god. Lastly, Behind this you see guilt. [2]
Bulimia Remedies: [2]
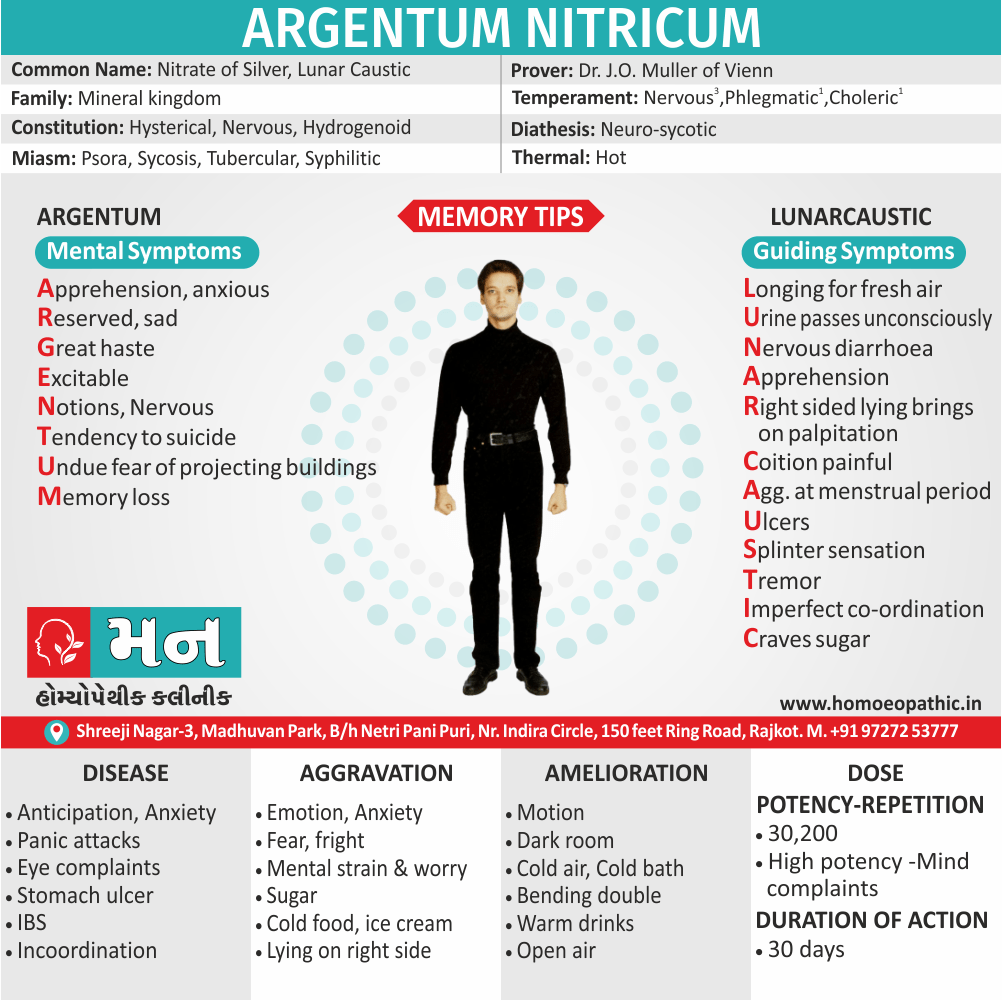
Argentum nit:
Binging especially with chocolate, fixed ideas, impulsive behaviour, anticipation, overriding impulses for certain foods, chocolate, salty foods, they will eat a whole box of chocolates until they get sick.
Carcinosin:
Obsessive compulsive disorder. Moreover, Perfectionism, fear of becoming fat, fear of rejection. Etiology-abuse, grief or fears, often related to weight.
Ignatia:
Perfectionism, fear of becoming fat, fear of rejection. Additionally, Hysteria-loss of control of emotions, fainting. Etiology-grief or big disappointment, often related to weight.
Medorrhinum:
Ups and down in the person’s energy, very outgoing for 2 or 3 days than wiped out for several days and with that their diets fluctuate from good to binging. Bulimia also with alcohol and drugs.
Natrum mur:
Often indicated remedy in anorexia, a lot of guilt. Fear of being rejected, hurt easily. Very self-conscious of their weight.
Pulsatilla:
Fear of being abandoned and unloved. Fixed ideas about food, their weight, they gain and lose weight easily, eat and binge to console themselves, binges out of loneliness, or depression, then they get guilt and fear about it and then suppress it.
Staphysagria:
Binging out of guilt, depression. Poor self-confidence and worthlessness. It is out of self-denial, they do not deserve that -lemon meringue pie so they suppress their desire for it, and then binge on it. [2]
Diet & Regimen
Diet & Regimen of Eating Disorder
- Encourage weight gain
- Take well balanced diet
- Take part in social activities
- Avoid talking about weight & food
- Avoid over exercise
Do’s and Dont’s xxx
Tab Content
Terminology xxx
Tab Content
References
Reference
- A Short Textbook of PSYCHIATRY 7th edition by Niraj Ahuja / ch 12.
- Homeopathy in treatment of Psychological Disorders by Shilpa Harwani / ch 15.
- Eating disorders – Symptoms and causes – Mayo Clinic
- Eating Disorder Examination (eatingdisorders.com)
- Eating Disorder Diagnosis: Tests, Screening, and Criteria (verywellhealth.com)
- 3 Simple Ways to Prevent Eating Disorders – wikiHow
FAQ
Frequently Asked Questions
What is Eating Disorder?
Eating disorders are actually serious and often fatal illnesses that cause severe disturbances to a person’s eating behaviors.
Homeopathic Medicines used by Homeopathic Doctors in treatment of Eating Disorder?
- Arsenicum alb
- Carcinosin
- Hyoscyamus
- Ignatia
- Natrum mur
- Phosphoric acid
- Platina met
- Pulsatilla
- Sepia
What causes Eating Disorder?
- Frequently appear during the teen years or young adulthood
- Affect both genders
- Women are 2½ times greater than among men.
- Distorted sense of body image
What are the symptoms of Eating Disorder?
- Dramatic weight loss
- Wearing big or baggy clothes
- Obsession with weight
- Obsession with continuous exercise.
- Frequent trips to the bathroom immediately following meals
- Visible food restriction and self-starvation.
- Visible bingeing and/or purging.
- Isolation
Give types of Eating Disorder?
- Anorexia Nervosa
- Bulimia Nervosa
- Compulsive Overeating or Binge Eating Disorder
- Obesity
- Psychogenic Vomiting
Also Search As xxx
Frequently Asked Questions (FAQ)
XYZ
XXX
XYZ
XXX
XYZ
XXX
People found Homeopathic Clinic For XXXX by searching for
XXX
People found Homeopathic Doctors for XXXX by searching for
XXX
People found Homeopathic treatment for XXXX by searching for
XXX